Who can get IMTP?Primary IMTP is more commonly seen in middle aged female dogs, especially Cocker Spaniels, German Shepherds, Poodles, and Old English Sheepdogs. Unfortunately, although it is more common in these breeds, it can happen at any age, any sex, and any breed. Secondary IMTP can occur in any pet as there is a secondary condition like infection, cancer, or sepsis causing the IMTP. What is IMTP?
Comments
Unfortunately, our fuzzy little one’s livers cannot handle many of the medications that humans take. This is one of the many reasons why all medications, prescribed by a physician or over-the-counter, must never be shared with your pet. AcetaminophenBoth cats and dogs are unable to process acetaminophen (Tylenol®). As little as 1 or 2 tablets of acetaminophen can cause problems for pets. Acetaminophen causes death (necrosis) to the cells of the liver. As the cells of the liver (hepatocytes) die, pets may start showing signs of sickness. Signs that may be noticed include vomiting, lethargy, decreased appetite, and icterus (yellowing of the skin and eyes).
Who can get IMHA?The bad news? Any breed can be diagnosed at any age. Both dogs and cats can be diagnosed with IMHA. Cats are definitely not as common, but they can still get it. Some risk factors reported include:
What is IMHA? Immune Mediated Hemolytic Anemia (IMHA) is also known as Auto-Immune Hemolytic Anemia (AIHA). Both names are for the same disease. It is when the body’s immune system sees erythrocytes, or red blood cells (RBCs), as a foreign invader needing to be destroyed. The immune system no longer recognizes the RBC’s as belonging to the animal and starts breaking down the cells. This causes severe anemia, or low red blood cell counts. As you can imagine RBC’s are essential for life. They are important for the body as they carry oxygen from the lungs to the rest of the body. That is why when a patient is anemic, they are weak and have exercise intolerance because the cells in the body are not getting the oxygen needed to perform their tasks. The term for decreased oxygen in the blood is hypoxemia. In dogs and cats we check the packed cell volume, or PCV, to tell us how anemic the patient is. Normal for dogs and cats is typically between 35%-55% and 25%-45% respectively. What this means is of the blood circulating in the body, how much is RBC’s and how much is fluid. The body likes to have a normal percentage of RBC’s and fluid concentrations. To know what the PCV is, a small blood sample is place into tubes and spun down with a centrifuge. This can take anywhere from 8-12 minutes. After the sample has been centrifuged the blood has separated into solids (blood cells: predominantly RBC's) and the liquid, plasma, portion of the blood. See the pictures below. General Diagnostics to RunWhen your veterinarian suspects an immune mediated disease it is important to screen for any underlying diseases that can stimulate the immune system. Common diseases that can trigger an auto-immune response is cancer, and tick borne diseases.
Cancer screening include thoracic radiographs (chest x-rays), abdominal ultrasound, and full blood work including a chemistry and CBC. Tick borne disease testing looks for these common infections that can trigger an immune response:
Feline Specific:
Have you been tasked with monitoring at least one aspect of your pet's vitals?
Are you confused about where to start? Well, don’t panic... Here is how to accomplish it!! Monitoring vitals is a crucial part of each and every visit to your Veterinarians' office. Occasionally, there are times where you will also need to keep an eye on your pet's vitals at home. So let us break this down to make this a manageable task, and therefore more likely to get accurate measurements to help your Veterinarian! What are Vitals?
Technically, they are specific clinical measurements of one's temperature, pulse (heart rate) rate, respiratory (breathing) rate, and blood pressure. These clinical measurements are checked each time you bring your pet to see their doctor. We take these measurements so routinely that you may not even realize it is being done!
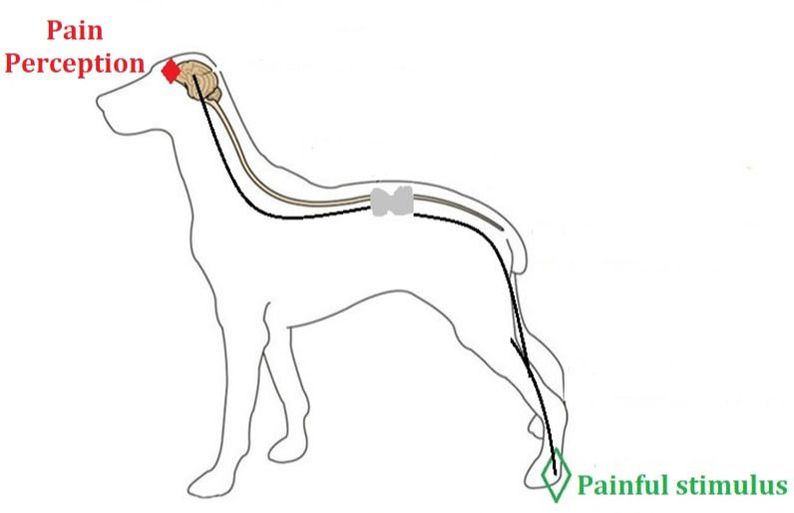
TemperatureOver the last several years, the concepts of pain and pain management have become more widespread within the veterinary community. There has been a growing need to understand the physiology of pain, identify the signs of pain, and be able to provide pain relief to our patient population, in order to enhance our patients’ comfort and overall quality of life. The International Association for the Study of Pain defines pain as, “an unpleasant sensory and emotional experience associated with actual or potential tissue damage”. Pain starts through stimulation of pain receptors (called nociceptors) that are present within the central nervous system, and are responsible for causing a pain response. Pain is a sensory process (nociception) that involves a series of electrical events, starting at the site of tissue injury, which then conveys signals to the brain, and results in the perception of pain (Figure 1). Perception is how the animal feels pain and is a subjective experience. Signs of pain can be classified as either behavioral or physiological. Behavioral signs are usually recognized first as they occur outwardly and are more readily observed. Physiological signs are systemic in nature, and therefore require a more hands on approach for assessment. Both behavioral and physiological signs are summarized below (Table 1).
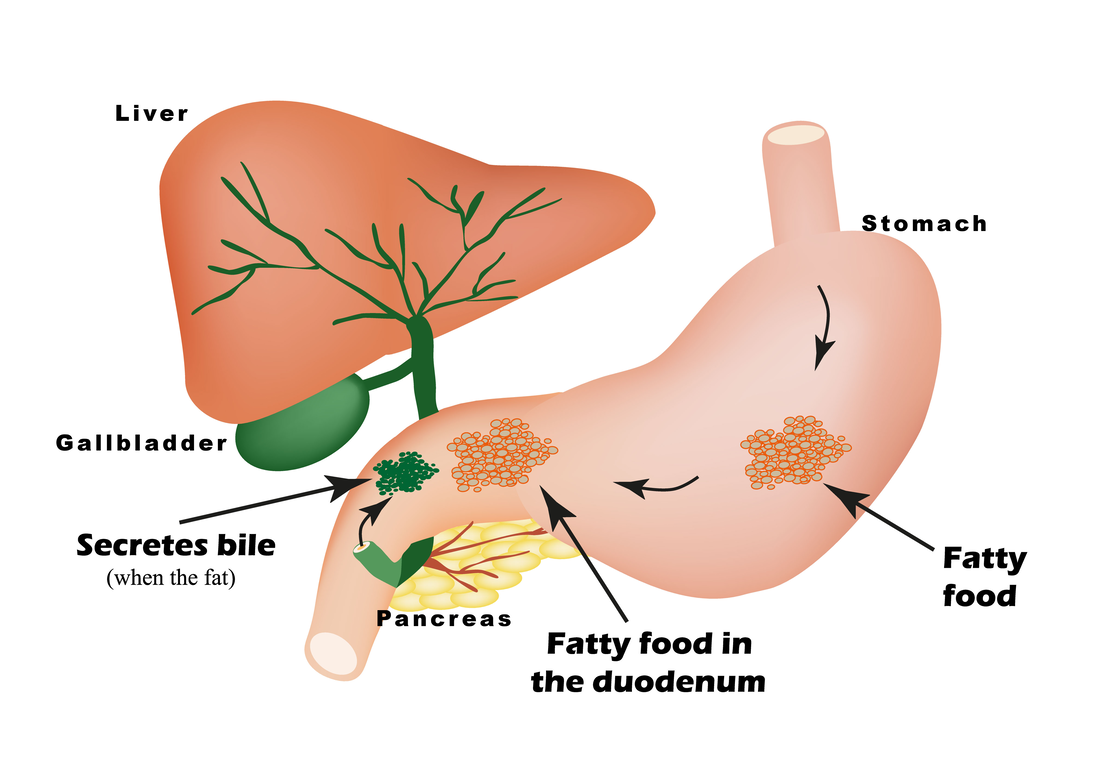
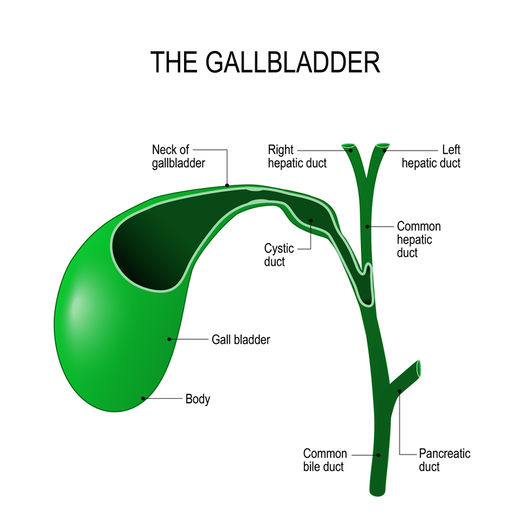
A little organ tucked in that helps with digestionNestled between the lobes of the liver, lies the gallbladder. It serves as a reservoir for bile. As the liver produces the bile, it moves through canals (called canniculi) through the liver until it travels through the hepatic duct and into the gallbladder. Once food has entered the stomach, a chemical cue stimulates the gallbladder to release the bile. The bile flows from the gallbladder through the common bile duct and is secreted into the stomach to facilitate digestion of the meal. The gallbladder is part of the gastrointestinal system and is important in digesting food. Occasionally, problems can arise! Problems can stem from obstructions, neoplasia (cancer), or stones, to name a few. Obstructions can be caused by an inflamed and swollen pancreas (pancreatitis) compressing the common bile duct, gall stones blocking the duct completely, or cancer. Or, the bile itself can become too thick to travel through the common bile duct and can back up in the gallbladder itself and cause pain and discomfort. Sometimes the bile can become a mucous ball that does not leave the gallbladder, this is called a mucocele and can be an emergency situation. Addressing problems affecting the gallbladder quickly is important because if they are left untreated, they can cause serious complications. If you notice your pet not eating as well as they used to, vomiting, or if your pets skin, eyes or gums begin to turn yellow, please seek veterinary care immediately. If your veterinarian recommends removal of your pets gallbladder, do not fret! Cats and dogs can live long and healthy lives without it and not suffer any complications! AuthorAshley DiPrete, RVT, VTS (SAIM) is a Registered Veterinary Technician practicing in California and obtained her Veterinary Technician Specialty in Small Animal Internal Medicine in 2016. She is the co-founder and a contributing author for InternalMedicineForPetParents.com. Visit her author page here. We're Growing!We're excited to be creating the Diseases section of the website and getting it up and running for you to enjoy. We're working hard to make sure the information is there for you for the diseases you want to know more about. The Hematology page is pretty well set up, so go check it out here. You'll get a sneak peak into what our plans are for all the body systems. The goal is to build up the Diseases section to be a resource for anyone looking for more information about a particular body system or disease process that is internal medicine related. A quick warning: If you see this adorable worker pug, the page isn't quite ready yet. Check back and hopefully we'll have it up and ready for you soon! We'd love your feedback as we go along, so if you read a particular page and you still have questions please email them to us because if you've got questions, we're betting someone else may have the same question! Send an email to us by following the link here. As always, if you'd like to stay up to date with what's going on join the newsletter for weekly updates and get a copy of our Weekly Medication Tracker, a downloadable PDF you can use to track your pets medications and daily habits. AuthorYvonne Brandenburg, RVT, VTS (SAIM) is a Registered Veterinary Technician practicing in California and obtained her Veterinary Technician Specialty in Small Animal Internal Medicine in 2016. She is the founder of InternalMedicineForPetParents.com. For more about Yvonne visit her author page here. Getting an Over Active Immune System to Chill Auto immune or immune mediated diseases are those diseases where the immune systems has malfunctioned and is attacking its own body. The immune system is too sensitive, it's hyperactive, it is responding to things inappropriately. What are some of the common immune mediated diseases? Immune Mediated Hemolytic Anemia, Immune Mediated Thrombocytopeina, Evans Syndrome, Immune Mediated Neutrophilia, Panniculitis, and Immune Mediated Polyarthritis. In the case of most of these diseases, the immune system has wrongly tagged the body's cells with an antigen tag that labels it as a foreign invader. Normally these antigen tags are a good thing. In a normal immune system when a virus, bacteria, or other foreign organism invades for the first time the immune system has to first recognize the organism as being harmful. Once the immune system establishes this, it remembers the organism by creating an antibody (a type of protein in the blood) specifically for the antigen so the next time the antibody runs into the antigen, the immune system can respond quicker and better. The immune system catalogs the antigens with the corresponding antibodies. The more antibodies for a specific disease floating in the blood stream, the easier it is to find that invading antigens. These are measured with antibody titer levels. The higher the titer, the more the immune system can patrol the body. Think of the antibodies as police, if there are more cops on the beat, crime goes down. But, if there aren't enough police officers, bad things can spread quickly and invade the surrounding neighborhoods. If the body incorrectly tags a cell within its own body as being bad, then the immune system produces more antibodies for these 'invaders' and more of the body's normal cells are attacked. What can we do to stop the body attacking it's own cells? We suppress the immune system. A suppressed immune system means it is sluggish to work, or it doesn't respond at all to antigens. In order to do this we used certain medications. Be aware that close monitoring of your pets blood is required during the initial phase of treatment, and it is very common for doses to change frequently. I highly recommend using a spread sheet to keep track of medications to help prevent missing or doubling doses. I also found a pill dispenser to be very helpful to make sure nothing gets missed. Filling the dispenser once a week can save time throughout your week, and keep you sane. Drugs Commonly UsedWhat is an immune mediated disease? First of all, an Immune Mediated disease and an Auto-Immune disease are the same thing and the terms can used interchangeably. These diseases are ones in which the body is attacking its own cells. Instead of the immune system only attacking foreign invaders to keep the body healthy, somehow a malfunction occurred and the body labeled its own cells as being bad and is killing them. DiagnosesWe don't fully know what causes the body to attack itself, but some of the theories being tested currently include:
Immune mediated diseases can be extremely frustrating to determine if they are a primary or secondary immune reaction, but it is crucial for prognosis (long term outcome) of the pet. Unfortunately, diagnosing primary immune disease is a diagnosis of rule outs. What this means is the veterinarian must test for, and rule out, all the other causes that can set off the immune system. We'll cover this is in a different post. Treatment |

Ready to Work Together?
Thank you!You have successfully joined our subscriber list. This website is NOT a substitute for veterinary care with a veterinarian. We recommend you follow the advice and treatment plan as prescribed by your veterinarian, and only after discussing anything found on this website with your veterinarian, with their approval, implementing advice found here.
Most of the information on this site is free for you to read, watch or listen to, but Internal Medicine for Pet Parents is also a business. So please expect hyperlinks to be affiliate links in many cases, where we receive a small percentage of sales if you wish to purchase. We only recommend tools, books and services that we use, or people we know personally. Integrity and authenticity continue to be of the highest importance to us. Read the privacy policy here. We hope you find the site useful! Thanks – Yvonne and Ashley Check us out on Facebook!
Categories
All
Archives
October 2019
|










 RSS Feed
RSS Feed